This post was born out of discussions with my doctor friends, who frequently struggle with “revolving door” patients. The kind of people you discharge knowing you’ll be seeing them in a few weeks, maybe even a few days. Individuals who grudgingly accept treatment, as though intent on remaining sick. Those who fail to follow medical advice, despite the pain and risks they then live with. Questions arise as to whether we should treat these patients at all, whether the resources are justified when they seem determined not to look after their own health.
“Non-compliance” has a very punitive ring to it. We comply with authorities, with court orders and sanctions. It suggests the existence of an external control and an absence of choice. The somewhat softer “non-adherence” is perhaps something all of us can relate to. Which amongst us have not been entirely adherent to medical advice? Perhaps we failed to complete a course of medicine, drank whilst on antibiotics or missed a few doses. This kind of non-compliance is one of the highest rated frustrations for doctors, but is very common.
Who is more likely to be non-compliant?
In a review of 102 papers, Jin, Sklar, Oh and Li (2008) found that those who do not comply are more likely to be male, younger, single, to have a lower level of education. Those who have a cognitive impairment (e.g. dementia), a mood disorder or use substances were also found to be more likely to be non-compliant. The complexity of treatment regime, level of medical knowledge, quality of relationship with the prescriber, and stigma attached with the treatment were also highlighted. However, it may not always be as clear “why” an individual is non-compliant, and attention needs to be given to the paradoxical nature of the behaviour.
Beliefs impacting on compliance
Research suggests that cognitive factors may lie behind this “everyday” non-compliance: faulty and inaccurate beliefs that guide behaviour. Patients may believe that the treatment will be ineffective or there will be minimal consequences to non-adherence. They may believe that they are not “truly” ill or that the treatment will impact them negatively. They may believe that the disease is uncontrollable or have religious beliefs regarding illness, or that an alternative method that will help them more.
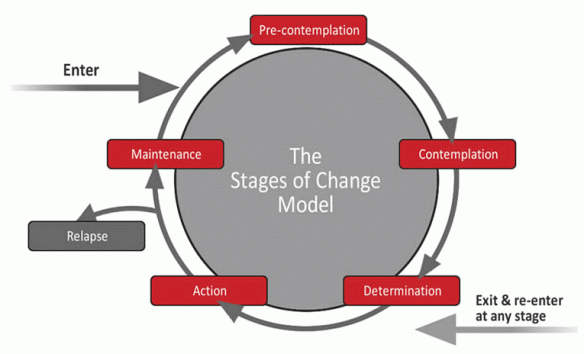
Readiness to change
Thinking of the “stages of change” model, many patients may still be at the ‘pre-contemplation’ stage in relation to changing their behaviour. They will need support, education and counselling to progress to a point where they feel capable of change. When medical emergency forces a patient to receive medical treatment, they may still not be ready to engage in change, despite professionals escalating the situation on their behalf.
A good relationship with a professional will be needed to open up a dialogue in which it may become apparent that patients hold these beliefs. In many cases education may be enough to shift the belief, but this will need to be provided in a respectful manner so it can be well received. Motivational interviewing techniques have been used successfully to help a patient to identify discrepancies between their behaviour and their goals.
But what of people with more “severe” forms of non-compliance? Those who seem to actively avoid treatment and seem to exacerbate their condition?
I’m reminded of Tom Main’s classic paper, “The Ailment”. Written in 1957, it still feels so relevant now. The paper discusses the frustration healthcare professionals experience when, despite their best efforts, patients do not get better.
“Only the most mature of therapists are able to encounter frustration of their hopes without
some ambivalence towards the patient, and with patients who do not get better, or who even get worse in spite of long devoted care, major strain may arise. Those who attend the patient are then pleased neither with him nor themselves and the quality of their concern for him alters accordingly, with consequences that can be severe for both patient and attendants.”
Encountering this type of frustration can lead to professionals using particular coping mechanisms that may be unconscious (defences). These include developing detachment and cynicism towards the patient or throwing more and more energy in, in a frantic attempt to “cure”. These tactics are ultimately unsuccessful and this is where burnout can occur.
This paper reminds professionals to be mindful of how a patient’s non-compliance or lack of progress affects us and to be aware of when we start to act out in these ways, to the detriment of both the patient and ourselves. We will not be able to “fix” everyone and, like they say in motivational interviewing, sometimes we need to “roll with resistance”. If someone is not ready to change, we cannot successfully force change on them.
The reasons why someone might maintain their sickness or actively reject help may be very complex but important to acknowledge. It may feel contradictory: why would someone present to hospital only to resist the support they are given. Why do some patients seem so unaware of the role they have played in their sickness? Why do some patients respond some hostility towards health professionals, who only intend to help them?
Secondary gain in sickness
For some their may be a benefit to adopting a “sick-role”. Whilst some intentionally cultivate or fake medical symptoms for gain, there may be others for whom this is not a fully conscious process. This behaviour may have been reinforced by others or remaining sick may (counter-intuitively) seem “safer” than the alternative. They may experience their emotions through physical symptoms (“somatization“) or have found being “ill” the only way they know how to seek care.
Learning to trust and tolerate “help”
Some patients may have a very poor “relationship to help”. For them a health professional who offers care is not a source of comfort. They may have learnt that they need to be independent and cannot rely on others. Perhaps those in role where they should have helped them (such as parents, teachers) have neglected or abused them. Receiving help may be associated with intolerable feelings of weakness and vulnerability. These feelings and experiences may place the individual in conflict when they are forced into a situation (e.g. onset of illness) where they are “required” to be helped, and part of them may continue to fight against this.
The legacy of trauma
For some individuals, especially those who have suffered significant abuse and trauma, they may hold beliefs deep inside that they fundamentally do not deserve help, that they aren’t worth the care given (see this example here). Perhaps they believe that they will (or should) die and try to resist attempts to sustain their lives. This may not reflect a conscious intention to kill themselves, but in their neglect of themselves they shorten their lives. They may have no sense of a future in which they can be “well”.
Cutting off from pain
As professionals can detach themselves from their difficult feelings from their patients, methods of separation and denial, these defences may too be at play in the patient. Being ill and requiring support may bring up very painful feelings, perhaps related to past experiences. They may hold a very real fear of their illness and the consequences. Denying the existence of the illness, the need for help and their own role in getting better may be a way of keeping a distance from these painful feelings. (This article is an interesting look at non-compliance in chronically ill adolescents and looks at some of the conscious and unconscious drivers.) Although the word “denial” is often used in popular culture, in its true meaning the individual is not consciously trying to “deny” the issue, but unconsciously does so to avoid intense emotional pain. Attempting to confront “denial” head-on is unlikely to be helpful, and there may be more of a benefit to trying to stand alongside the patient and understand where the need for such a defence may have come from. 
Countering frustration with compassion
Understanding some of the reasons behind this “pathological” non-compliance will not instantly lead to an answer as to how to help the individual. Understanding someone’s story and experiences, including their experiences of being cared for and receiving help, may shed some light on current behaviour and also help to maintain empathy in the face of very frustrating behaviour. Patients may struggle to trust professionals and need time to develop a relationship in which some of this information could arise. In some fast-paced environments such as acute medical wards, time pressures may limit this. There will not always be the opportunity to refer someone to mental health teams for assessment and begin the slow process of unpicking the complex factors contributing to their behaviour. As Main says, it may not be possible for us to help everyone, as much as we might like to. But creating space to consider of some of these potential factors may help to see the person behind the behaviour and facilitate the patient in having a positive experience of health professionals that may build their ability to engage in the future.
If you’ve found the content of this piece interesting I’d love to hear your thoughts! I’m putting together a follow-up regarding staff support and ways of supporting compassion/avoiding burnout in healthcare professions.